Rebuilding the Brain After a Stroke: A Comprehensive Guide
Stroke recovery is a deeply personal journey that blends medical care, targeted therapy, and daily routines that support healing. This guide explains how the brain changes after a stroke, why neuroplasticity matters, and which rehabilitation techniques can improve movement, speech, and thinking skills over time.
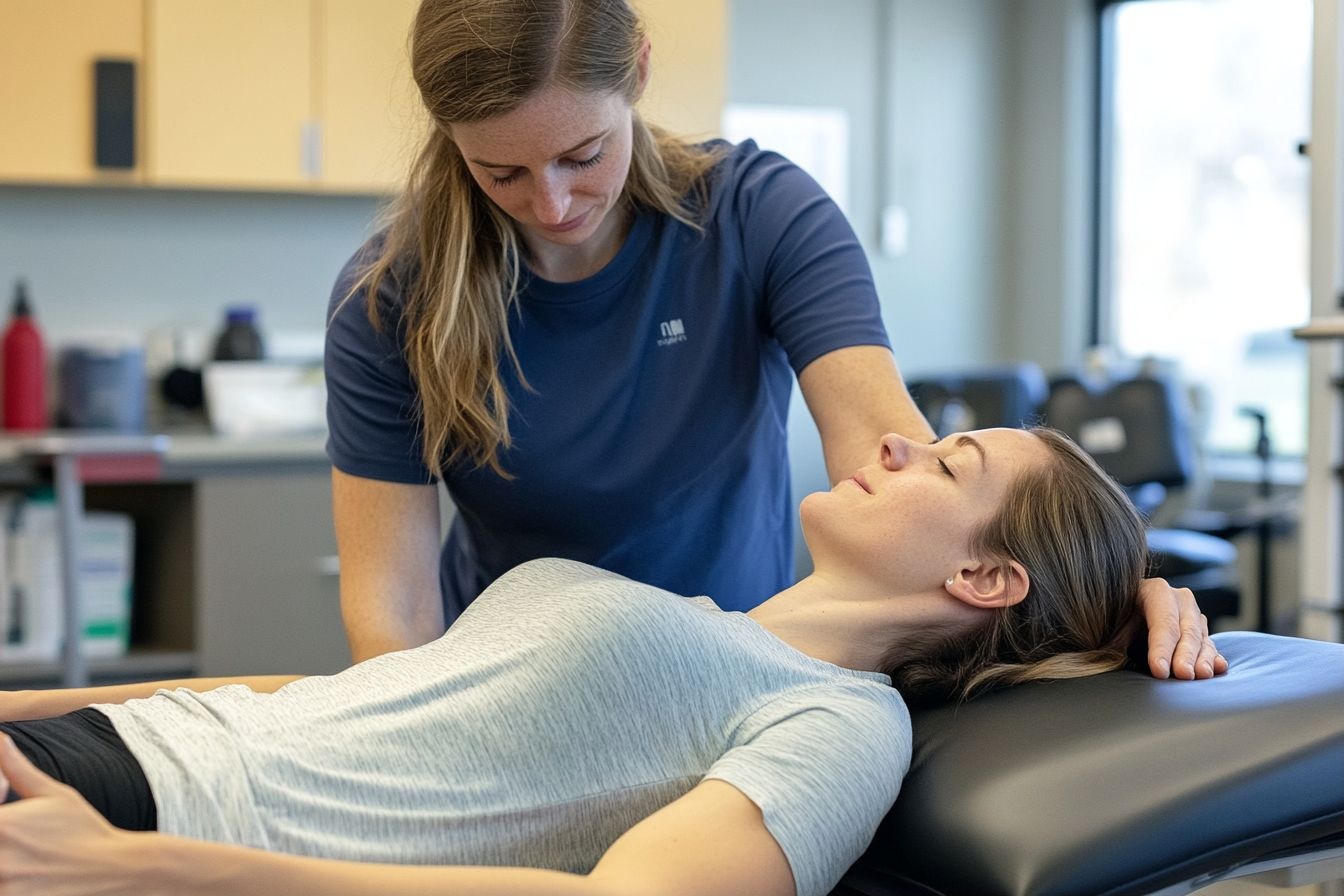
Stroke recovery involves careful timing, the right mix of therapies, and habits that encourage the brain to rewire. While each person’s path is unique, understanding what changes inside the brain and how to engage in consistent rehabilitation can make the process more structured and hopeful. Progress often comes in small steps, and it is shaped by the type of stroke, the areas affected, preexisting health, and the intensity of practice.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Understanding Stroke and Its Impact on the Brain
A stroke disrupts blood flow to parts of the brain. In ischemic stroke, a clot blocks an artery; in hemorrhagic stroke, a vessel ruptures and bleeds into or around brain tissue. Both can injure neural networks responsible for movement, sensation, language, vision, memory, and emotion. The symptoms you see after a stroke reflect which regions and pathways are affected and how severely.
Recovery unfolds in phases. The acute phase focuses on stabilizing health and preventing complications. In the subacute and chronic phases, rehabilitation aims to restore function or develop compensatory strategies that support daily life. Some abilities may return spontaneously as swelling decreases and surviving cells resume activity. Many gains, however, emerge through structured practice that strengthens usable pathways and builds new connections.
Neuroplasticity: The Brain’s Ability to Heal
Neuroplasticity is the brain’s capacity to reorganize by forming and strengthening connections. After a stroke, nearby and connected regions can take on new roles. Practice that is task specific, repetitive, progressively challenging, and meaningful to the person encourages these adaptive changes. In general, intensity matters: more high‑quality repetitions often lead to better outcomes, provided fatigue and safety are managed.
The first months after a stroke are often described as a period of heightened plasticity, but meaningful gains can still occur later with consistent effort. Aerobic exercise, adequate sleep, balanced nutrition, and managing conditions like high blood pressure and diabetes can support brain health. Avoid learned nonuse, where an affected limb is neglected; guided use under supervision can help reengage weakened networks. Both restoration of function and smart compensation—such as using assistive devices—are valid routes to independence.
Physical Rehabilitation Techniques
Physical therapy targets movement, strength, and balance. Therapists often use task‑oriented training, gait practice with body‑weight support, balance exercises, and functional electrical stimulation to activate weak muscles. Constraint‑induced movement therapy may be used for some people with arm weakness, encouraging use of the affected limb during structured tasks. Simple tools like mirrors can aid symmetry and awareness, while graded resistance and flexibility work help with joint protection and endurance.
Occupational therapy focuses on daily activities such as dressing, bathing, cooking, and work tasks. Interventions blend motor practice with problem‑solving strategies, home modifications, and energy conservation. Adaptive equipment—grab bars, raised seats, non‑slip mats, one‑handed tools—can reduce risk and increase independence. Therapists may suggest environmental changes and connect you with local services in your area for home safety assessments.
Speech and language therapy addresses aphasia, dysarthria, and apraxia of speech, as well as swallowing difficulties. Treatment can include language drills, conversation practice, alternative communication methods, and breath‑voice control. Cognitive rehabilitation may work on attention, memory, executive function, and visual‑spatial skills using structured exercises tied to real‑world tasks.
Technology can complement therapy. Robotic devices, virtual reality scenarios, and tablet‑based apps provide engaging, repeatable tasks and objective feedback. Remote or hybrid models can extend access between clinic visits. Home exercise programs, customized by your therapy team, help maintain intensity; short, frequent practice sessions are often more sustainable and effective than occasional long ones.
Daily routines support recovery. Aim for a consistent schedule that alternates focused work with rest to avoid fatigue. Prioritize sleep hygiene, hydration, and a nutrient‑dense diet. Gentle aerobic activity—such as walking within safe limits—can improve cardiovascular health and cognition when approved by a clinician. If mood changes, anxiety, or post‑stroke fatigue arise, mental health support and peer groups can be valuable; many hospitals and community organizations offer groups and educational resources.
Safety remains central. Review medications and risk factors with your medical team. Learn the signs of recurrent stroke and establish a plan with family or caregivers. Home fall‑prevention steps—clear walkways, adequate lighting, and supportive footwear—lower risk. If you live far from specialized centers, ask about community rehabilitation programs and telehealth options offered by local services.
Setting goals and measuring progress
Collaborative goal setting helps align therapy with what matters most, such as walking to the mailbox, returning to a hobby, or preparing a simple meal. Goals are commonly structured to be specific, measurable, achievable, relevant, and time‑bound. Therapists may use standardized measures—like gait speed, balance tests, arm function scales, or language assessments—to track change over weeks and months. Small improvements, such as an extra minute of standing tolerance or clearer word retrieval, are meaningful markers that your plan is on course.
Gradually increase complexity as skills improve. For movement, that could mean progressing from sitting balance to standing, then to stepping and community mobility with or without aids. For language, it might progress from naming objects to structured conversation and problem‑solving. Periodic reassessment allows the team to adjust intensity, add technology, or shift toward community reintegration and maintenance.
The role of caregivers and the care team
Recovery is rarely a solo effort. Family members and caregivers often help coordinate appointments, reinforce exercises, and support motivation. Training for safe transfers, cueing strategies, and communication techniques can reduce stress for everyone involved. Your interdisciplinary team—medical providers, nurses, physical, occupational, and speech therapists, psychologists, and social workers—can help you navigate resources, transportation, and financial assistance programs that may exist in your area. Clear communication about goals, progress, and barriers keeps rehabilitation personalized and safe.
Conclusion
Rebuilding the brain after a stroke is an ongoing process shaped by biology, timing, and daily choices. While outcomes vary, consistent, meaningful practice and supportive routines can foster change at any stage. Understanding how stroke affects the brain, using neuroplasticity‑informed strategies, and applying the right mix of physical, cognitive, and communication therapies can help restore function or build effective workarounds that support independence and quality of life.




