Understanding Genital Psoriasis and Its Common Warning Signs
Genital psoriasis is a form of psoriasis that affects sensitive skin areas and can be confusing or concerning for those experiencing it for the first time. Because symptoms may resemble other skin conditions, it is often misunderstood or overlooked. Genital psoriasis is not contagious, but it can cause discomfort, irritation, and emotional stress. Learning to recognize common warning signs, understanding how it differs from other conditions, and knowing when to seek medical guidance can help individuals feel more informed and prepared. This guide explains the basics in a clear, respectful way, focusing on awareness and general understanding rather than diagnosis or treatment.
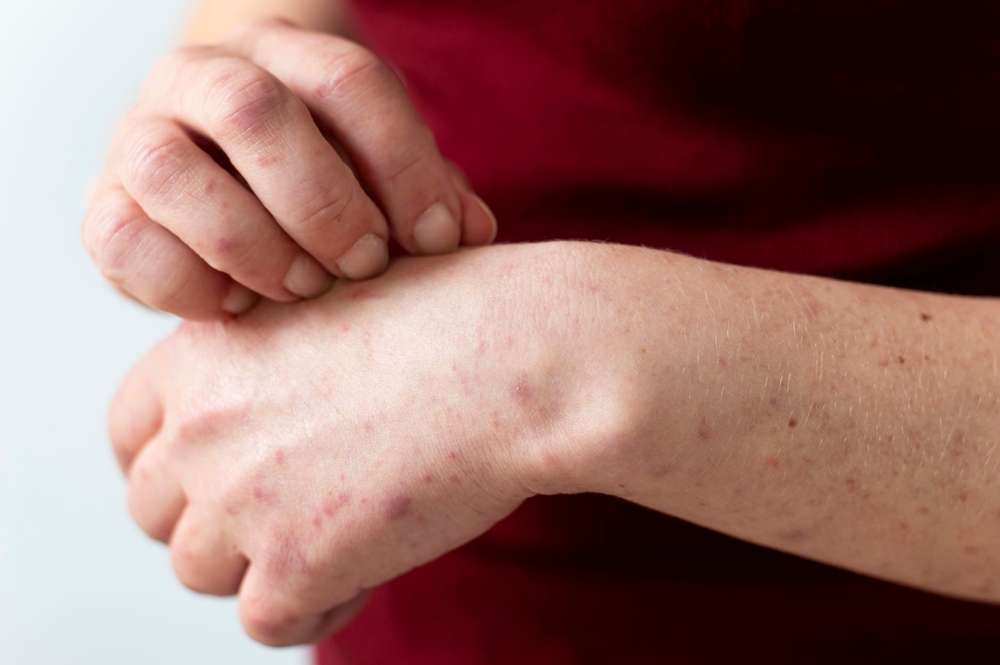
Genital psoriasis is a chronic autoimmune skin condition that affects the intimate areas of both men and women. Unlike psoriasis that appears on other parts of the body, genital psoriasis presents unique characteristics and challenges due to the sensitive nature of the affected area. This condition can significantly impact quality of life, relationships, and emotional well-being, making early recognition and proper management essential.
What Genital Psoriasis Is and How It Differs From Other Skin Conditions
Genital psoriasis is a form of inverse psoriasis that occurs in the genital region, including the pubic area, genitals, and surrounding skin folds. Unlike typical plaque psoriasis that creates thick, scaly patches, genital psoriasis usually appears as smooth, red, inflamed areas without the characteristic silvery scales. The warm, moist environment of the genital area prevents the formation of typical psoriatic scales, making it appear different from psoriasis elsewhere on the body.
This condition is often mistaken for other skin issues such as yeast infections, sexually transmitted infections, or contact dermatitis. The lack of scales and the location can make diagnosis challenging, requiring careful examination by healthcare professionals. Unlike fungal infections, genital psoriasis typically doesn’t respond to antifungal treatments and may worsen with certain topical medications not designed for sensitive areas.
Common Warning Signs and Sensations to Be Aware Of
The warning signs of genital psoriasis can vary between individuals but typically include persistent red, inflamed patches in the genital area. These patches may appear smooth and shiny, lacking the typical scales associated with psoriasis elsewhere on the body. Patients often experience itching, burning, or stinging sensations that can range from mild to severe.
Other common symptoms include pain during urination, discomfort during sexual activity, and general tenderness in the affected area. The skin may appear cracked or fissured, particularly in areas where skin rubs together. Some individuals report a feeling of rawness or soreness that persists despite attempts at relief with over-the-counter treatments.
Factors That May Trigger or Worsen Symptoms
Several factors can trigger or exacerbate genital psoriasis symptoms. Friction from tight clothing, underwear, or physical activity can irritate the sensitive skin and worsen inflammation. Stress, both physical and emotional, is a well-known trigger for psoriasis flares throughout the body, including the genital area.
Hormonal changes, particularly those occurring during menstruation, pregnancy, or menopause, can influence symptom severity. Certain medications, infections, and injuries to the area may also trigger flares. Poor hygiene or excessive washing with harsh soaps can disrupt the skin barrier and worsen symptoms. Additionally, sexual activity may cause mechanical irritation that can trigger or worsen existing psoriasis.
When to Seek Professional Medical Advice
Immediate medical attention should be sought when symptoms persist for more than a few days or worsen despite basic care measures. If over-the-counter treatments for common conditions like yeast infections don’t provide relief within a week, professional evaluation is necessary. Any unusual discharge, severe pain, or signs of secondary bacterial infection warrant prompt medical attention.
Individuals should also consult healthcare providers if symptoms interfere with daily activities, sexual function, or emotional well-being. Early diagnosis and treatment can prevent complications and improve quality of life significantly. Healthcare providers can perform necessary tests to rule out other conditions and develop appropriate treatment plans tailored to the sensitive genital area.
| Treatment Option | Provider Type | Typical Approach | Estimated Cost Range |
|---|---|---|---|
| Topical Corticosteroids | Dermatologist | Mild to moderate strength creams | $30-150 per prescription |
| Calcineurin Inhibitors | Dermatologist | Non-steroidal topical treatment | $200-400 per prescription |
| Phototherapy | Specialized Clinics | UV light treatment sessions | $75-200 per session |
| Systemic Medications | Rheumatologist/Dermatologist | Oral or injectable treatments | $1,000-5,000 monthly |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Building Awareness and Managing Skin Health Carefully
Understanding genital psoriasis and recognizing its warning signs empowers individuals to seek appropriate care and manage their condition effectively. While this chronic condition can be challenging, proper medical supervision and treatment can significantly improve symptoms and quality of life. Regular follow-ups with healthcare providers ensure treatment effectiveness and allow for adjustments as needed.
Maintaining good genital hygiene with gentle, fragrance-free products and wearing loose, breathable clothing can help minimize irritation. Open communication with healthcare providers about symptoms, concerns, and treatment responses is crucial for optimal management. With proper awareness and medical support, individuals with genital psoriasis can maintain healthy, comfortable lives while managing their condition successfully.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.